The Blog
- Acne
- Maskne
- Melasma
- Pigmentation
- Hyperpigmentation
- Eczema
- Covid-19
- Rashes
- Covid-19 Vaccine
- Fillers
- Scars
- Botox
- Neurotoxins
- Skin
- Rosacea
- Seborrhea
- Anti-aging
- Skin Cancer
- Chemical Peels
- Allergies
- Infection
- Skin Tags
- Medical Care
- Dry Skin
- Skin Care
- Skin Care Tips
- Acne
- psoriasis
- Dandruff
- Impetigo
- Hair
- Intertrigo

Dermatology is a complex field encompassing disorders of the hair, skin, and nails. Did you know there are thousands of dermatological conditions all with variants and different presentations? As you can imagine, with such a vast number of conditions, there can be many myths. Myths are a widely held, but false belief or idea. In today’s era of social media, it is not surprising that myths can spread like wild wildfire! Some common dermatology myths that we hear daily range from sunscreen application to acne cure all’s to miracles for hair loss. Our goal is to discuss and help debunk some of these myths.
“My shampoo is making my hair fall out!” – This is a myth!
This is a myth. It is not uncommon for patients to stop shampooing their hair when they are experiencing hair loss. This scenario can be upsetting for patients, as they want to wash their hair more frequently, but are fearful that washing their hair will cause more shed. The truth is that the hair that falls out in the shower is destined to fall. When hair becomes wet, it tends to clump together and creates the illusion of more hair shed. Showering and shampooing do not increase hair shed or alter the cycles of the follicles. In fact, a healthy scalp is vital in preserving healthy hair. When the scalp is not washed properly, dead skin and debris build and actually puts more pressure on the follicles. It is safe to shampoo at least every other day and even daily. We have yet to find an article proving shampooing causes shedding and encourage you to join me in showering freely!
“I am too young to lose my hair!” – Thankfully this is a myth!
This is a myth. It is not true that only older people can lose their hair. Many hair losses are secondary to underlying genetics, and hair loss can rear its ugly head at any point in life. Genetics does not discriminate, and both men and women can be affected equally. Genes are complicated, and patterns can be unrecognized, especially in females. At our office we have seen 13-year-old boys with thinning, as well as young women in their 20s with receding hairlines. For many patients with genetic hair loss, regrowth is possible, and, fortunately, there is a range of treatments available. These options include oral medications, such as spironolactone, as well as topical systems and procedures such as Platelet Rich Plasma or Keravive. Treatments are continuously changing with updates in research and technology, and there are always more options coming onto the horizon to combat this frustrating class of diseases. We are very passionate about helping those with hair loss and realize the impact it can have on self-esteem. We would love to discuss all your options with you further and encourage our patients to know they are not alone.
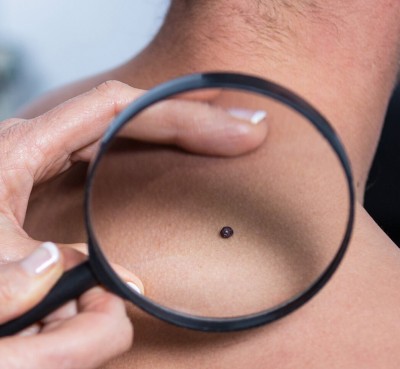
One very common myth we often discuss in our practice is that, “All raised lesions are melanoma.”
Thankfully, this myth is false. Melanoma is an aggressive form of skin cancer that can lead to metastasis and death if left untreated. Melanoma is frequently characterized by a new or changing lesion. Melanoma most often arises on its own as a “new lesion.” However, there are occurrences where it can arise from a previously existing atypical mole. Many types of lesions are raised on the skin and are completely benign. In fact, it is not uncommon for harmless moles to become raised slowly over time. Raised moles or dermal moles arise from the deeper layers in the skin. They are often soft and frequently have soft hairs growing through them. These are typically reassuring findings.
“Every dark lesion is melanoma.” – This is another myth.
This is a myth. It is not uncommon for patients to fear dark lesions; however, the reality is that there are plenty of dark lesions that are completely harmless. Moles, for example, as well as other common lesions, such as seborrheic keratoses, can have varied pigmentation. These pigmentations can vary from tan to very dark-brown and even almost black. These presentations can also vary per ethnic background. It is not uncommon for those with darker underlying skin tones to make darker moles and freckles. A lesion that is commonly concerning for patients and often mistaken for “melanoma” is a seborrheic keratosis. While seborrheic keratoses can be very dark and occasionally have irregular pigmentation, they are a common, benign type of skin growth that typically occurs in later adulthood. They are not related to moles, but they are completely harmless. We often refer to them as “wisdom spots” for many of our patients. The golden rule in dermatology is that monitoring all lesions on your skin is always key! Darker lesions that are one toned and with an even border are often reassuring findings, but if you feel like you have noticed changes, trust yourself. Sampling these lesions is a quick and easy process. We are always happy to offer reassurance and further care if needed. The bottom line is we have your back (literally) and are happy to take a peek!
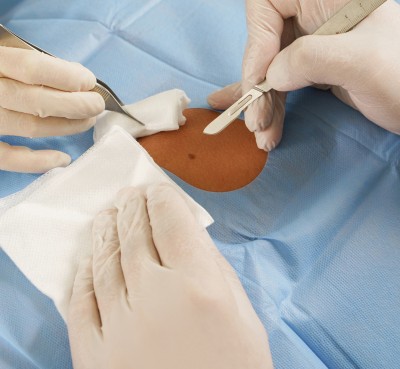
“Aren’t all skin cancers the same?” – This could not be more false!
This is another myth. Did you know there are three common types of skin cancer? Melanoma is the worst, however, thankfully it is the least common type. The most common type of skin cancer is a basal cell carcinoma (BCC). These are typically characterized by shiny, pink patches or bumps that occur in high sun-exposed locations, such as the chest, ears, and nose. This type of skin cancer is highly treatable and is typically slow-growing. The second most common type of skin cancer is a squamous cell carcinoma (SCC). Like BCCs, these are also characterized by chronic sun exposure; however, they can also arise from the HPV virus, which is the same virus that commonly causes warts. This type of skin cancer typically arises as a rough, pink, and sometimes tender lesion of the skin. There are multiple subtypes of BCCs and SCCs and many treatment options available. The treatment will depend on the type and stage of cancer, and treatment options range from topical chemotherapy cream to surgical excisions, such as MOHS micrographic surgery. It is important to treat all forms of skin cancer, as there is a risk of progression and metastasis if left untreated.
“I’ve heard air helps wounds heal better.” – This is not true!
The misconception that air will help wounds heal is a myth. It is a common old wives’ tale that “drying out” wounds helps expedite the healing process. We frequently see our patients walking around with a thick, dry scab over their biopsy or surgical site at follow-up. The truth is that air tends to create dry wounds that impede the natural healing process. Scabs can act like a brick wall to a healing wound. It is difficult to penetrate a brick wall, and it is similarly difficult for wounds with scabs to properly heal. Rather than drying out your wound and exposing it to air, try keeping it moist and covered. Vaseline is your friend! It is hypoallergenic and affordable. Chances are if you know someone who works in dermatology, you will know how much we cherish this emollient. We encourage all family, friends, and patients to stock up on Vaseline. It is invaluable and helps keep a wound moist while preventing scabs. After applying Vaseline, I also encourage you to apply a bandage until the site is fully healed. You will not believe how much faster your wound will heal, and you may also be surprised how much better your scar looks!
“I know how important cleaning a wound with hydrogen peroxide is.” – This is false!
This is also false. While we are on the discussion of dry wounds, I wouldn’t be a good dermatology PA without discussing my dislike of hydrogen peroxide. Another very common thought is that hydrogen peroxide keeps wounds clean. While good in theory, it is also extremely drying! Remember, when it comes to wound healing, moisture is key. Truly, normal water (or sterile water after an excision!) and soap are all you need! Keep that wound clean, apply a bandage, and go about your day. Your wound will heal, and you will be thrilled with how fast it’s gone!
“I can’t believe some people shower daily, isn’t that awful for your skin?” – This is a myth.
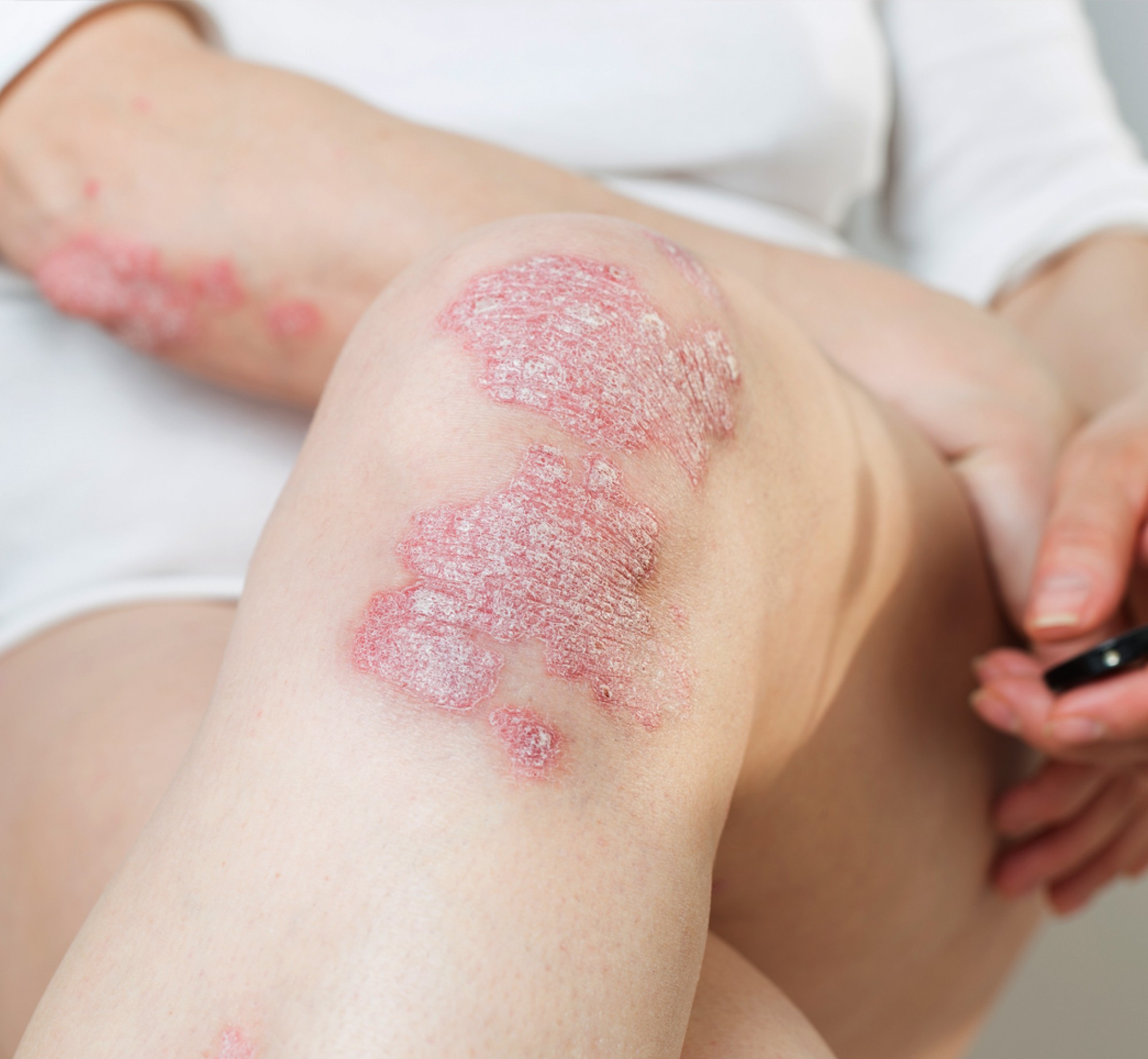
This is another common myth. Showering can be done daily, and, in fact, we encourage many of our patients to shower every day. The fear of dry skin is at the heart of showering daily. Eczema is very common dry skin condition and affects children, adults, and all races and sexes. Dry skin is enemy number one regarding eczema, and the winter months can be difficult due to a lack of humidity. Showering is actually very important regarding eczema, as it helps keep rates of bacterial infection lower. A lukewarm shower daily is what we recommend for all our eczema-prone patients. We also recommend using a very gentle hypoallergenic soap and moisturizing from head to toe right after showering for even better penetration into the skin.
“I have heard that supplements and diet can drastically improve my acne” – This is not true.
Another myth. Social media is a common source of misinformation, and this is also false. We often encounter patients questioning the acne miracles they heard about on Facebook and Instagram. A very common misconception regarding acne is diet. To be honest; the literature is very mixed regarding the benefits of diet changes and improving acne. Some reports have shown that inflammation can contribute to acne, and inflammation is not uncommon when individuals sensitive to gluten do not follow a gluten-free diet. Again, this is not true for everyone and may not benefit someone without gluten sensitivity. The bottom line is the majority of patients benefit the most from a consistent medical-grade skincare regimen. Vitamins are also an equally tricky subject. Many people, for example, believe that vitamin B is beneficial in treating acne. Vitamin B has quite the opposite impact on acne and can worsen or exacerbate acne in many patients. Each patient is different, and not all acne is created equal. We enjoy tailoring our regimens for each patient and encourage you to discuss further with your dermatology professionals.
“Now that the weather is cooler, I have been hiking with friends. I am itching, but I was definitely not bitten by an insect! No one else in my group has one bite.” – This is a myth!
This is another myth. This is a scenario we encounter frequently in dermatology. A patient will present with itchy, swollen, pink bumps on their skin, typically with a central indent. It is not uncommon for the patient to have a history of being outdoors, however, this is not always the case and you can be bit indoors. The insect bite may not be witnessed and this often can be confusing for patients and is easy to assume that the bumps cannot be secondary to bug bites.
Insects are interesting, as they have an affinity to certain people. This affinity can be related to a patient’s unique scent or even the color of their clothing. People can also react very differently to insect bites. For some people, it is negligible and they don’t even notice. While for others, a bite can result in itching or swelling and even hives. If you are unsure about a rash or a bite, do not hesitate to consult with your dermatologist. A dermatologist can help you manage exaggerated reactions, as these can develop into a skin infection after repeated cycles of itching and scratching.
“What type of insect bit me? Was it a spider?” – This can be difficult to determine and it is a myth that all bites are secondary to spiders.
In most circumstances we cannot identify the insect, unless the patient obtains the insect in a container for us to analyze. Not all insect bites are secondary to spiders. Spider bites tend to be mostly venomous and have more dramatic presentations.
“Do I have bed bugs? I am terrified all these bites are from bed bugs” – Thankfully this is typically a myth as well
In cases of bed bugs, there is usually a history of travel or being in an unfamiliar place. We always advise our patients to thoroughly check their bedding area in an unfamiliar residence or hotel, and to assess the seams of bedding and the mattress itself. If you are in doubt, turn off all lights for one hour and make sure you still have white-colored bedding to allow for easy analysis of any crawling insects. It is very important that if you do have bed bugs that you exterminate them completely from your luggage because they are difficult to manage if they get into your household. General prevention is always key in the prevention of insect bites. Over-the-counter insect repellents have been examined by the FDA and are safe. For those who are hesitant to apply these insect repellents, we encourage oil of citronella, which is a natural extract and reasonably priced. It can be applied to trigger points on the body that generates heat to diffuse the scent that is offensive to insects. To reiterate, you can be the only person who has been bitten by insects in your group. You could also be the only person who reacts in a special way to insect bites. Do not hesitate to consult with your dermatologist if you are in doubt.
Myths are not uncommon, and we encourage you to do your research before following what you read on social media.
There are many common myths in dermatology, and the golden rule is every patient is different and individual. We always encourage our patients to ask questions, and we would encourage you to research what you read online prior to buying into a new fad or trend. Evidence-based practice is based in science, and we use these recommendations when choosing treatment plans for our patients. If you are ever in doubt, know that your dermatologists are always happy to help and guide you!