The Blog
- Acne
- Maskne
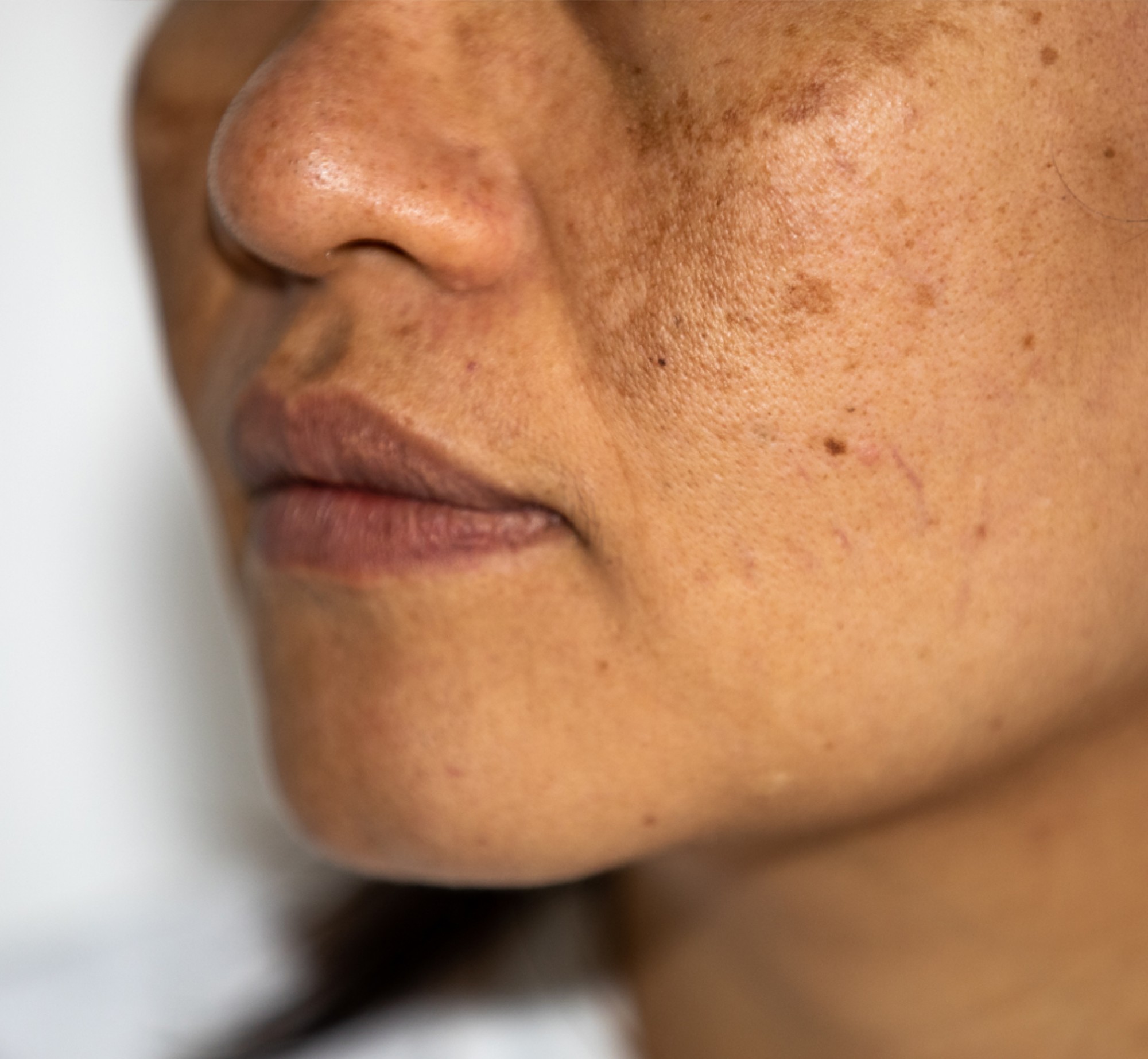
- Melasma
- Pigmentation
- Hyperpigmentation
- Eczema
- Covid-19
- Rashes
- Covid-19 Vaccine
- Fillers
- Scars
- Botox
- Neurotoxins
- Skin
- Rosacea
- Seborrhea
- Anti-aging
- Skin Cancer
- Chemical Peels
- Allergies
- Infection
- Skin Tags
- Medical Care
- Dry Skin
- Skin Care
- Skin Care Tips
- Acne
- psoriasis
- Dandruff
- Impetigo
- Hair
- Intertrigo
Rosacea, seborrhea and acne are three of the most common facial rashes we see in dermatology. It can be tricky to spot the differences between these facial rashes, and in some cases these rashes can coexist together making the treatment plan even more challenging. We will go through common features of each of these rashes and how to spot the difference.
First up, let’s talk ACNE.
Almost all of us will experience some form of acne throughout our lives. Acne typically affects adolescents but can actually occur at any age. There are forms of acne that even affect infants.
What are the defining features of Acne?
What separates acne from other facial rashes are comedones. “Comedones” are clogged pores and are often referred to as whiteheads (closed comedones) or blackheads (open comedones). Acne also presents with inflamed lesions (i.e. papules and pustules), and can even present with deep cystic lesions on the skin which feel like very firm and tender nodules under the skin.
Acne can affect the face, chest, back, neck and sometimes more extensively over the body. Acne lesions can often lead to scarring and dark marks on the skin even long after the active acne has resolved. That is why it is so important to prevent and control acne to prevent these permanent scars and marks.
What causes Acne?
There are many different risk factors that can contribute to developing acne on your skin.
- Age: Acne can occur at any age but predominantly occurs in adolescence. This is likely influenced by hormonal change around puberty as well.
- Hormones: Hormone fluctuations can trigger acne flares. Hormones fluctuate throughout our life, but especially during puberty and during pregnancy or menopause for women. There are also certain medications that can influence hormones, such as birth control pills or corticosteroids.
- Organisms On Our Skin: We all have bacteria and yeast that live normally on our skin. When the balance between these organisms becomes shifted, this can lead to acne breakouts and inflammation on our skin. The bacteria, P. acnes, and the yeast, Malessezia, have been shown to cause acne breakouts when they become overgrown.
- Genetics: There is no “acne gene” persay. However, you may inherit traits that make you more prone to developing acne, i.e. oily skin texture, or increased inflammatory markers in the skin.
- External Contacts: Oily or greasy substances on your skin can lead to clogged pores and, in turn, result in acne. It is important to use products that are oil-free on your face, that includes face cleanser, lotions, makeups and sunscreens. It is also important to change out your pillow case frequently as this can hold on to oil from our face and hair and continue to clog pores while we sleep.
- Occlusion: Friction or pressure on your skin can also lead to acne. This is especially relevant with athletes who wear head gear, helmets or pads. However, friction against your skin can also be caused by everyday items such as constant use of a cell phone against your cheek, or wearing a backpack for extended periods of time.
How is Acne treated?
First and foremost, it is important to start a regular topical facial routine to keep the skin clean and prevent excessive dirt and oil on the skin. This means washing your face morning and night with a hypoallergenic, fragrance free skin cleanser such as Cerave foaming facial wash or Cetaphil oil-reducing wash. After washing, you can apply your topical acne treatments, then apply an oil-free non-comedogenic facial moisturizer.
There are numerous topical acne products available OTC such as benzoyl peroxide, adapalene, salicylic acid, and azelaic acid just to name a few. There are even more topical options available with a prescription from your dermatology practitioner including topical antibiotics such as clindamycin, prescription grade retinoids, and numerous combination topicals for an easier routine.
Oral antibiotics are used commonly for inflammatory acne and to control acne flares. For some females who experience hormonal acne there are hormonal options such as spironolactone or birth control pills. Isotretinoin is an oral medication that is reserved for very severe and cystic acne.
The many treatment options available for acne can be very overwhelming for patients trying to manage their symptoms on their own. In general, if you are experiencing acne it is best to consult with a dermatology practitioner to guide you on the best topical maintenance plan for you.
Next up: Rosacea!
Are you red and rosy constantly on your face? Do you feel a warm sensation on your cheeks or neck sporadically throughout the day? Is it super difficult to control your “acne” even in your 40s, 50s or even 60s? If you answered yes to any of these questions you may have a condition called Rosacea!
Rosacea is a chronic inflammatory condition that affects the facial skin and sometimes the eyes. It has been historically thought of as a condition that only affects those with fair skin from European descent. It has even been coined “the curse of the Celts” owing to its European predominance. However, it does affect skin of color as well and may be underdiagnosed among these individuals. It usually occurs between the ages of 30 and 60 years old, but can occur at any age.
What does Rosacea look and feel like?
Patients with rosacea generally have redness through their mid face that may be persistent or may wax and wane. In patients with darker skin toned, “redness” may present with purple, grey or even blue undertones in the mid face.
Some patients with rosacea can have inflamed acne-like lesions and pustules that occur as well. Superficial blood vessels especially around the nose and inner cheeks is another common sign of rosacea.
Patients with rosacea tend to have very sensitive skin and may report stinging and burning on their skin, especially in response to makeups, sunscreens, or facial creams. Some patients may have very dry, flaky and irritable skin while other patients with rosacea may feel that their skin is excessively oily especially through the T zone.
“Flushing” can occur at random or in response to specific triggers and feels like a warm and tingling sensation accompanied by a wave of redness covering the skin of the face and neck.
There is also a more severe subtype of rosacea called Phymatous rosacea in which chronic inflammation leads to thickening of the skin. This most commonly affects the nose but can actually occur on any ares of the face.
Ocular rosacea is a subtype of rosacea in which inflammation of blood vessels in the eyes leads to redness, burning and irritation of the eyes. This often coexists with the skin symptoms but can occur on its own.
Not all patients with rosacea will present with the same symptoms - some patients may have all the characteristics while others may just have one feature, such as flushing.
What causes Rosacea?
There are multiple theories about what causes rosacea that we will explore below. We do know that it is not related to acne but can often be misdiagnosed as acne if a practitioner is not careful.
• Inflammation:
We know that a person’s genetics plays a role in the development of rosacea. In general, it seems that patients have a genetic makeup that makes them more susceptible to developing rosacea at some point in their life. At an early age increased inflammatory factors in the skin have been noted in patients with rosacea. These inflammatory factors can contribute to prolonged vasodilation (i.e. dilation of blood vessels) that is perceived as redness in the skin. They also contribute to the formation of pustules in the skin.
• Blood Vessel Dysfunction:
Blood vessels in the top layer of the skin become dilated and allow fluid to leak out into the superficial layer of the skin. The blood itself can cause perceived redness, and this in turn drives additional inflammation and redness in the skin.
• Skin Mites:
All humans have a microscopic mite on our skin called Demodex folliculorum. This is a normal occurring organism that lives on our skin in the hair follicles, oil glands and eyelid glands. It has been noted that patients with rosacea have a significantly higher number of these organisms on their skin. Their role in rosacea is somewhat unknown but is thought to further drive inflammation in the skin.
• Environmental Factors:
There are multiple environmental triggers that can make rosacea much worse or trigger flares of rosacea. Spicy foods, alcohol, sun exposure, hot foods or beverages, caffeine, hot showers or hot environments, are the most common triggers of rosacea.
How is Rosacea treated?
• Avoid Triggers:
The first step in treatment for Rosacea is trying to avoid known triggers. That means wearing a daily moisturizer with SPF. And because of the sensitivity most Rosacea patients experience it is important to choose a product that is hypoallergenic and mineral based (i.e. contains zinc and/or titanium dioxide; avoid chemical sunscreens.) That also means avoiding hot and spicy foods, limiting alcohol and caffeine, avoiding hot showers/baths or other exposures that make your facial redness and flushing worse.
I tell my patients to keep a journal log around times of flares and record what you were doing and what you were eating or drinking prior to rosacea flares.
• Topical Treatments:
There are numerous topical treatments used for rosacea. They are considered the “first line” option for treatment. In general, most patients require a maintenance routine with at least one topical to control symptoms.
Topical antibiotics such as metronidazole or clindamycin are commonly used to reduce inflammation. There are other topicals such as Mirvaso or Rhofade that act on the blood vessels in the skin to push them away from the surface and constrict the blood vessels themselves to reduce redness in the skin. Soolantra is a topical that is used to reduce the mites on the skin, which in turn has anti-inflammatory and soothing effects on the skin.
These are just a few of the many topical options available for treatment of rosacea. For many patients, a combination approach is more successful than using a single topical cream.
• Oral Treatments:
Oral antibiotics, such as Doxycycline or Minocycline, are commonly used to control rosacea flares. Antibiotics are used to reduce inflammation in the skin and reduce overgrowth of bacteria on the skin. High dose antibiotics are not generally recommended for long term use due to antibiotic resistance and GI upset that can result from reducing the “good” bacteria in our gut. However, there is a product called Oracea which is a low dose doxycycline. At this low dose, it strictly serves as anti-inflammatory and does not actually kill bacteria in the GI tract making it a safer option for long term use. This option is available for patients with rosacea that is difficult to control with topicals alone.
• Vascular Laser:
Vascular laser is a great option to help reduce the appearance of blood vessels and redness on the skin. This can even be beneficial for patients with ocular rosacea as well. Most patients will require multiple rounds of treatments for best results and may require maintenance treatments over the years. In most cases, topical maintenance is still required to maintain control of rosacea in between laser sessions.
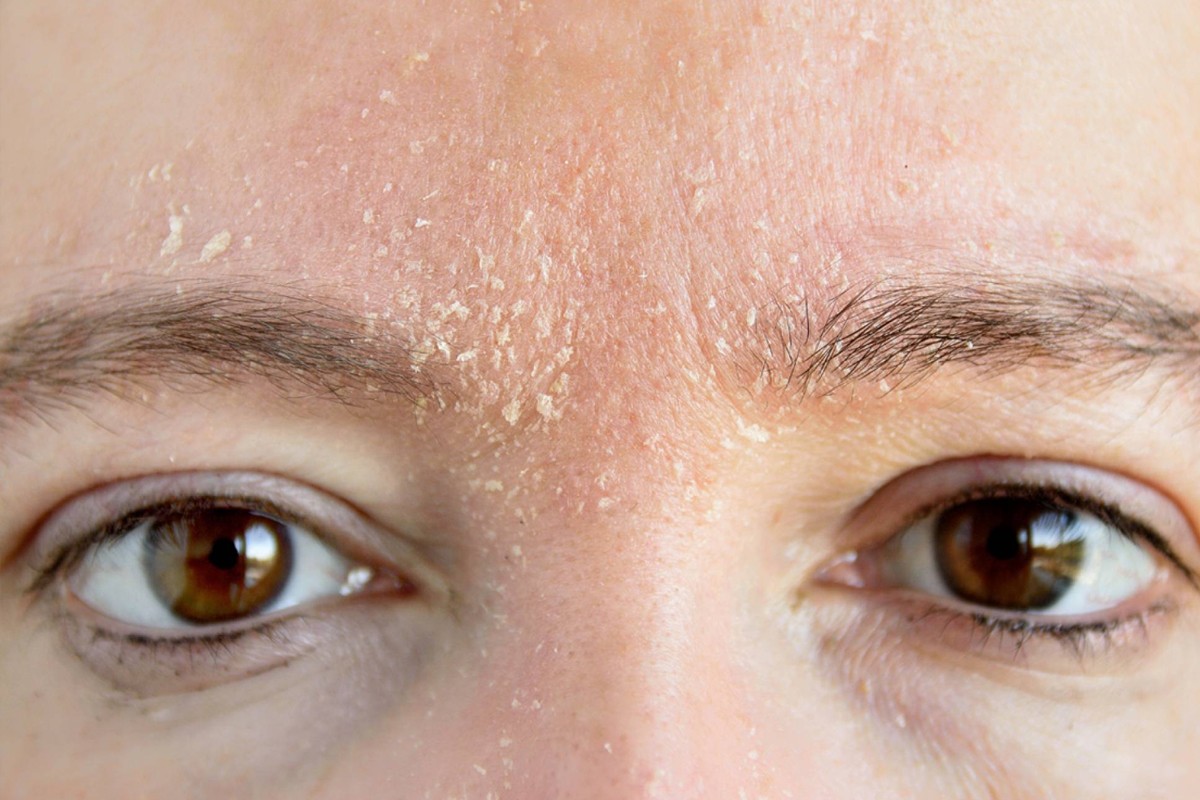
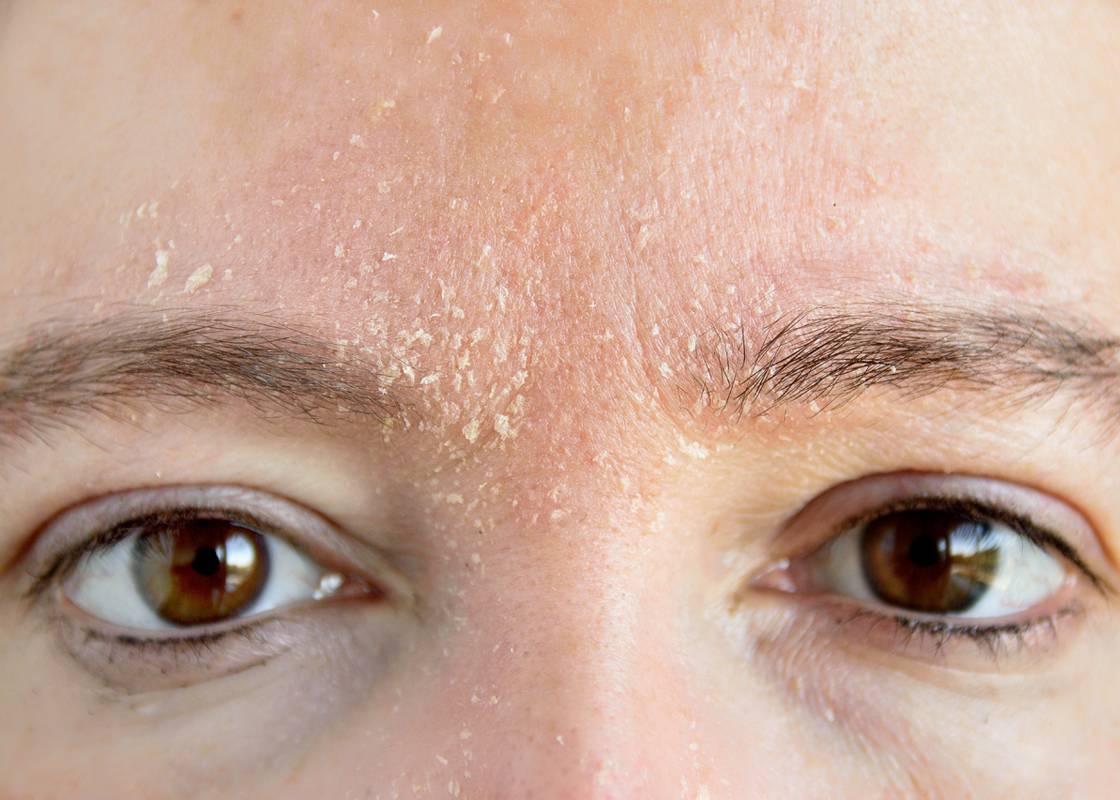
Last, but not least, let’s talk about Seborrhea.
Do you have persistent dry skin and scaling in certain areas of your face? Do you feel like your skin and hair is oily yet you constantly feel dry skin developing in certain areas of your scalp and face? You may have a common skin condition called seborrheic dermatitis.
What is Seborrhea?
Seborrhea, aka seborrheic dermatitis, is a common rash that affects areas on our skin that are rich in sebaceous glands, aka, oil glands - think face, scalp, chest, outer ears. It can affect infants in the form of “cradle cap,” but often affects adolescents and adults as well.
This condition typically presents with light pink to red patches with greasy scales and peeling. You will commonly see these patches in specific areas of the face such as the eyebrows, T-zone areas, eyelids, creases around the nose, or skin of the scalp or beard. Some patients will develop these rashes in the outer ears or mid chest as well. A defining feature of this rash is the distribution. You will not typically see this rash covering the entire face or affecting the arms or legs, rather it has a tendency to develop in these certain areas listed above.
What causes Seborrhea?
The cause of seborrheic dermatitis is not completely understood, but most dermatologists agree that there is an association with a common skin yeast called Malassezia. This yeast grows normally on all of our skin, however patients with seborrhea tend to have an overgrowth of this yeast. When this yeast becomes overgrown, it can lead to increased inflammation in the skin as well.
Patients with other underlying disorders or who are on certain medications can also be more prone to developing seborrheic dermatitis. Neurologic disorders including Parkinson’s disease, epilepsy, and spinal cord injury among others, have been associated with seborrhea. In addition, patients with Down Syndrome or any patients with immunosuppression can experience increased rates of seborrheic dermatitis. In addition, medications that lower the immune system such as chemotherapy and numerous psychoactive drugs such as lithium and buspirone have been associated with increased rates of seborrhea.
How is Seborrheic Dermatitis managed?
Seborrheic dermatitis often requires a maintenance topical routine to manage symptoms.
Topical ketoconazole is very commonly used for seborrheic dermatitis management. It is an anti-yeast medication targeted to reduce the amount of Malessezia on the skin. This is available in a cream or shampoo which can be used to your scalp or as a body and face wash.
There are many other shampoos that can be used as facial and scalp washes as well including selenium sulfide, coal tar, zinc pyrithione, and ciclopirox.
Topical steroids are generally used in the short term to control seborrheic dermatitis flares. Topical steroids are not ideal for long term use, as they have been associated with skin thinning, skin lightening and your skin can even become dependent on this medication if they are overused. Short courses are ideal, and it is always best to switch to non-steroidal options once the flare has been controlled.
Topical exfoliants can be beneficial in some patients to remove scales. These include salicylic acid, urea, lactic acid, among others.
Nonsteroidal creams such as pimecrolimus or tacrolimus can be used for patients who need a daily maintenance routine. These topicals are generally soothing and can be used to maintain control. You will need a prescription from your practitioner to use one of these creams.
For infants, treatment options are limited because of their very delicate skin. Regular washing of the scalp and face is important. Petroleum jelly can be applied to areas of thick scaling to help gently remove with a warm wet washcloth. If you are having trouble managing your infant’s cradle cap it is always best to consult with your practitioner to guide you on age appropriate treatment options.
Hopefully, you have learned a little about the common facial rashes that can affect your skin at all ages. If you are having trouble managing your symptoms it is always best to visit with your dermatology practitioner to develop a plan for your skin type. For most patients, combination therapies are most effective and provide the longest relief of symptoms. We hope to see you in our office soon for your skin care consultation!